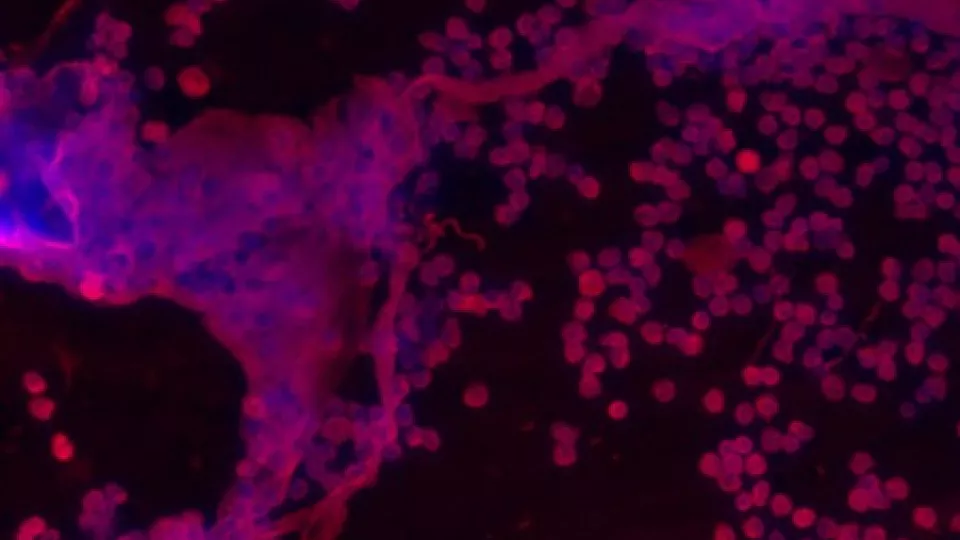
Seen here are the white blood cells (neutrophils) in the spinal fluid during bacterial meningitis. The nuclear material DNA is stained blue and proteins in neutrophils are stained red. The large aggregates as represented by overlapping areas of blue (DNA) and red (protein) portrays the extracellular DNA-protein networks called neutrophil extracellular traps (NETs). NETs are released as a defence response against invading bacteria in bacterial meningitis.
Our immune system has several important defenders to call on when an infection affects the central nervous system. The researchers have mapped what happens when one of them, the white blood cells called neutrophils, intervene in bacterial meningitis.
If there is an infection, the neutrophils deploy to the infected area in order to capture and neutralise the bacteria. It is a tough battle and the neutrophils usually die, but if the bacteria are difficult to eliminate, the neutrophils resort to other tactics.
“It is as though in pure frustration they turn themselves inside out in a desperate attempt to capture the bacteria they have not been able to overcome. Using this approach, they capture a number of bacteria at once in net-like structures, or neutrophil extracellular traps (NETs). This works very well in many places in the body where the NETs containing the captured bacteria can be transported in the blood and then neutralised in the liver or spleen, for example. However, in the case of bacterial meningitis these NETs get caught in the cerebrospinal space, and the cleaning station there is not very effective”, explains Adam Linder, associate professor at Lund University and specialist in Infectious Diseases at Skåne University Hospital.
Researchers observed, by using advanced microscopy; that the cerebrospinal fluid of patients with bacterial meningitis was cloudy and full of lumps, which proved to be NETs. However, among patients with viral meningitis, the cerebrospinal fluid was free from NETs. When captured bacteria get caught in the cerebrospinal fluid, this adversely affects the immune system’s work of clearing away bacteria and also impedes standard antibiotics from getting at the bacteria, says Adam Linder.
Would it be possible to cut up the nets so that the bacteria are exposed to the body’s immune system, as well as to antibiotics, making it easier to combat the infection? As the NETs consist mainly of DNA, the researchers investigated what would happen if you brought in drugs used for cutting up DNA, so-called DNase.
“We gave DNase to rats infected with pneumococcus bacteria, which caused bacterial meningitis, and could show that the NETs dissolved and the bacteria disappeared. It seems that when we cut up the NETs, the bacteria are exposed to the immune system, which finds it easier to combat the bacteria single-handed. We were able to facilitate a significant reduction in the number of bacteria without antibiotic intervention, says Tirthankar Mohanty, one of the researchers behind the study.
Before antibiotics, the mortality rate for bacterial meningitis was around 80 per cent. With the advent of antibiotics, the mortality rate quickly fell to around 30 per cent.
In the 1950s, Professor Tillett at the Rockefeller University in the USA, found lumps in the cerebrospinal fluid of patients with bacterial meningitis. Professor Tillett discovered that these lumps could be dissolved using DNase. This was effective in combination with antibiotics and reduced the mortality rate for meningitis from around 30 per cent to about 20 per cent. However, this treatment had side effects, as the DNase was extracted from animals and could therefore trigger allergic side effects.
“At that time, everyone was so happy about the antibiotics, they reduced mortality for the infections and it was thought that we had won the war against bacteria. I believe we need to go back and take up a part of the research that took place around the time of the breakthrough for antibiotics. We can perhaps learn from some of the discoveries that were then flushed down the drain”, says Adam Linder.
“The development of resistance in bacteria is accelerating and we need alternatives to antibiotics. The drug we use in the studies is a therapeutic biological product derived from humans and has already been approved for human use. They are not expensive and have also been tested against many different bacteria and infections. Bacterial meningitis is a major challenge in many parts of the world. In India, for example, it is a major cause of death among children, so there would be significant benefits there from using such a treatment strategy”, says Tirthankar Mohanty.
The researchers want to go on to set up a major international clinical study and use DNase in the treatment of patients with bacterial meningitis.
This research was supported by grants from: the Anna and Edwin Berger Foundation, the Swedish Government Research Grant (ALF, the Swedish Medical Society, SUS Funds (A.L), the Österlund Foundation (A.L.). The Crafoord Foundation, Stiftelsen Olle Engkvist Byggmästare, the Wallenberg Foundation Academy Fellow Program, the European Research Council starting grant and the Faculty of Medicine, Lund University.
Publication: Neutrophil extracellular traps in the central nervous system hinder bacterial clearance during pneumococcal meningitis
DOI: 10.1038/s41467-019-09040-0
Contact:
Adam Linder, associate professor, researcher, Division of Infection Medicine at Lund University and consultant at the Infections Clinic, Skåne University Hospital in Lund, Sweden
+46 46 171 130, +46 709 280233
adam [dot] linder [at] med [dot] lu [dot] se (adam[dot]linder[at]med[dot]lu[dot]se)
Tirthankar Mohanty, postdoc, research engineer, Division of Infection Medicine at Lund University, Sweden
+46 46 222 0720
tirthankar [dot] mohanty [at] med [dot] lu [dot] se