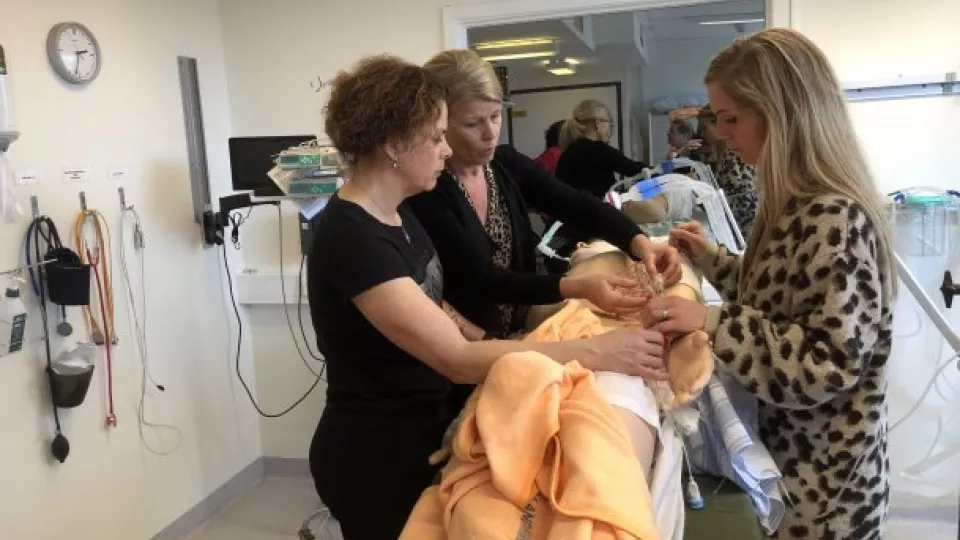
The short two-week course in intensive care for active nurses is well underway and was swiftly planned when the viral disease Covid-19 came knocking on the door. Lund University is collaborating on the course with Region Skåne and its centre for clinical skills and medical simulation, Practicum. The classes have approximately twelve nurses at a time, and a new class starts every week. Karin Samuelson is herself one of the members of teaching staff, as well as examiner. She says the participants are experienced nurses. However, in such a short course they are not expected to be able to operate advanced intensive care equipment, such as ventilators (or respirators, as they are also known).
“The course focuses on learning a few new skills and to feel confident in the intensive care environment. As they start to feel more confident, they may be provided with more tasks. In the course, they are given the opportunity to familiarise themselves with a ventilator and do some exercises with it. However, they are absolutely not given individual responsibility for it”, says Karin Samuelson.
In her research, she has studied how patients who were cared for in an ICU (intensive care unit) felt during treatment and after it was finalised. She has particularly focused on the memories of patients who were placed on ventilators. It showed that one in every three patients had memories of nightmares and hallucinations shortly after the ventilator support was discontinued. Two months later, eight per cent of patients suffered symptoms of post-traumatic stress disorder (PTSD), and just as many had symptoms of depression. The patients who were most worried during the period of care itself were also those who consequently suffered the most significant problems. It is vital, emphasises Karin Samuelson, to make the individual intensive care patient feel as safe as possible.
“We still do not know how significant the need for intensive care will become for Covid-19. However, even in times of pressure it is important to consider the experiences that my research is a part of, to ensure the safest possible intensive care environment and to follow up patients after they are discharged. Ensuring patients feel safe will become a challenge with the current ban on visitors and the requirements for everyone to wear a mask.”
Very anxious patients often require more sedatives. If the sedation is heavy, the patients find themselves in a sleep state. Karin Samuelson’s research shows that the most heavily sedated patients are the ones who find it most difficult to feel well after ventilator support is discontinued. Longer time on a ventilator is also a risk factor for subsequent problems. While other ICU patients often survive after just a couple of days on a ventilator, some Covid-19 patients are likely to have their ventilator support stretch out over several weeks.
“They will be more heavily sedated and, in addition, will require ‘difficult’ settings on the ventilator, i.e. settings that make it uncomfortable for the patient. When you come in with respiratory failure, you are breathing shallowly and panting and will fight against the machine setting that wants to make the breathing deeper and slower. This is why these patients may need to be sedated.”
The sleep does not become a solitary black gap in memory. Nightmares, hallucinations, anxiety and fear of dying are some of the experiences that patients have reported during Karin Samuelson’s interviews. Most memories of these things were reported by the patients who were cared for on a ventilator for the longest periods of time. Many patients remember some of what happened, however, the factual memories are mixed with dreams. Reality is interspersed in memories with things that are not real. Added to this is the anxiety already created by the difficult disease itself.
“There are many interacting factors that can make a difficult intensive care experience so hard. Firstly, you have faced the disease itself with great worry, anxiety and stress, both physiologically and emotionally. Then you are given lots of medication and sedatives. They are strong, potent drugs. You are not awake and your brain does not function as usual. It leads to a very cloudy existence in which you do not really know what is happening.”
Post-traumatic stress can persist for life if it remains untreated. The follow-up after intensive care that Karin Samuelson has been involved in developing is now available in many parts of Sweden. In Lund, the first step is for ICU staff to write a journal for the patient. It relates what happens, day by day, how the patient seems to have felt and if anything particular has happened. Brief and easy to understand, such as ‘today you had problems breathing for a while, so we did this.’
“You may remember something about not getting enough air, that you thought ‘I’m going to die!’. Afterwards, the diary can help to piece together your recollections. When the patient is moved out of ICU to an ordinary ward they are visited by an intensive care nurse who asks questions about the patient’s recollections of and state of mind after the intensive care. When needed, ICU staff can also provide support to staff on the ordinary ward to interpret the patient’s signals and state.”
Within a couple of months, a follow-up conversation is offered. At the follow-up visit any help the patient may need is identified, any referrals required are written up. Residual swelling and reduction in the mobility of the hands and feet may mean physiotherapy is required. It is not uncommon for a dietician to also be needed. Suddenly coffee tastes bad, the coffee that used to taste so wonderful! Moreover, all food may have a metallic taste, leading to the patient losing their appetite completely. For a patient who is already fragile it is crucial that this is addressed. The same applies to patients who continue to feel worried, anxious or depressed.
“So there will be quite a bit to do afterwards with regard to Covid-19. ‘Ordinary’ psychologists and doctors do not know how these patients are feeling after the intensive care treatment. A twenty year old usually recovers after just a couple of months. However, the average age of our ICU patients is 67. For patients of that age and older it often takes a year to recover. We have to focus on these patients, because afterwards they will be the only ones who can teach us what intensive care should look like.”
Karin Samuelson is now hoping that the follow-up of ICU care is scaled up in accordance with the demand. She also believes that the entire crisis situation should lead to change in the lean healthcare sector – so the management of future crises is improved.
“We have lost our way a bit with crisis management. Until the 80s and 90s, in healthcare we had stocks of food, equipment, ventilators… To have got rid of it all just to cut costs, that does not work. In addition, we do not have enough ICU beds, something we pointed out long before Covid-19 emerged. In Skåne, we have far below the average in Sweden and Sweden has below the average in Europe. After the crisis, I hope responsibility will be taken to ensure we are better equipped in the future.”